Curettage is commonly used for benign lesions such as seborrhoeic keratoses (Seb Ks) and warts. It can also be used for actinic keratoses (AKs), squamous cell carcinomas in situ (SCCis), and superficial BCCs.
It is important to be clear about the procedural intent for a curettage:
- The procedure can be used to remove benign lesions.
- It should not be considered a definitive treatment for invasive skin cancers. Success rates range from 60-90% when treating skin cancers, depending on the operator and location of the lesion. Judging the extent of the procedure is largely done by feel, so it is best performed by those with experience with the technique.
- It can be used to debulk more invasive skin cancers while waiting for definitive surgery to be undertaken or for those who don’t wish to proceed to definitive treatment.
Unfortunately, the tissue obtained does not allow for adequate histopathologic evaluation of margins and sometimes can even make diagnosis difficult. Therefore, it should only be used for selected cases where the lesion and the intent of treatment are clearly understood.
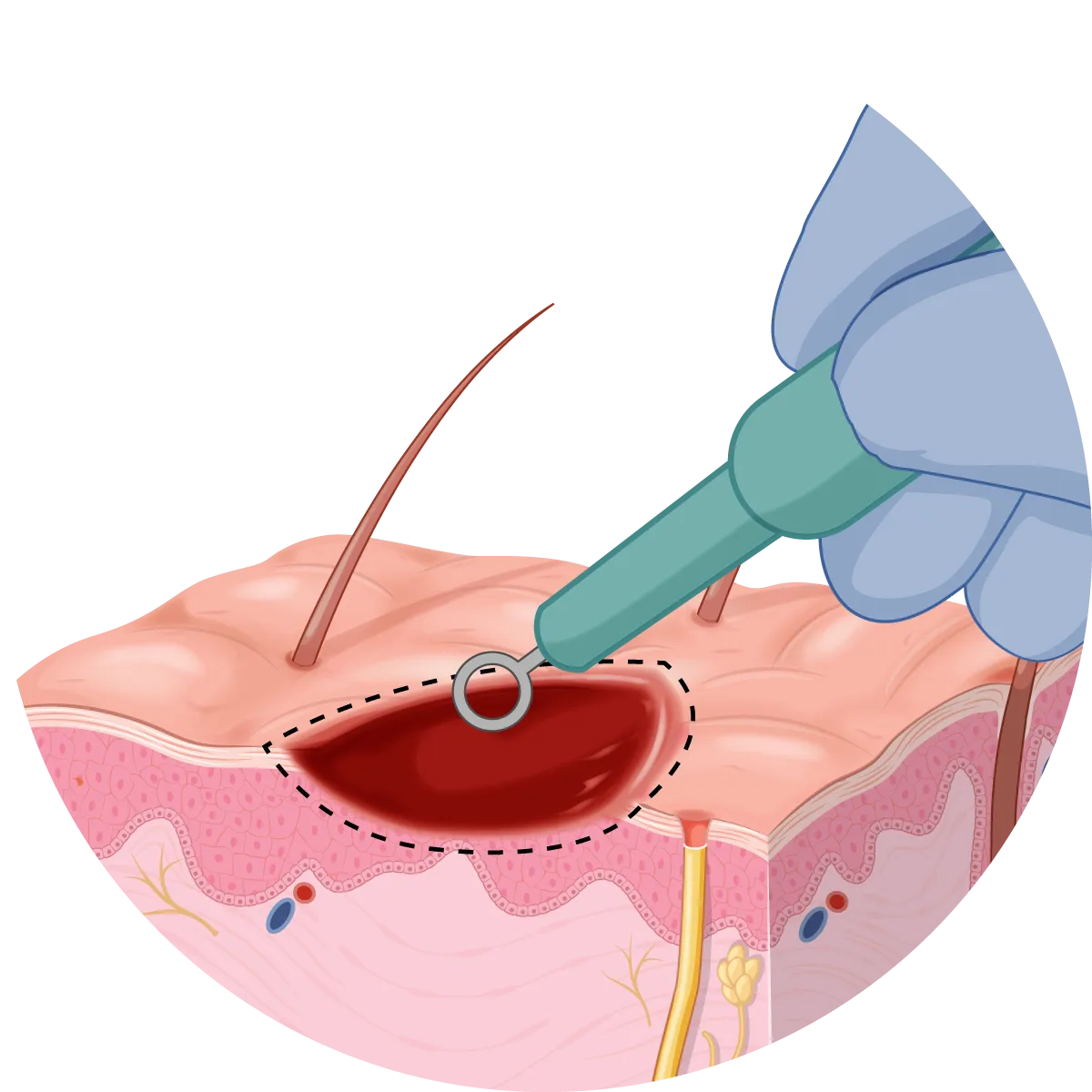
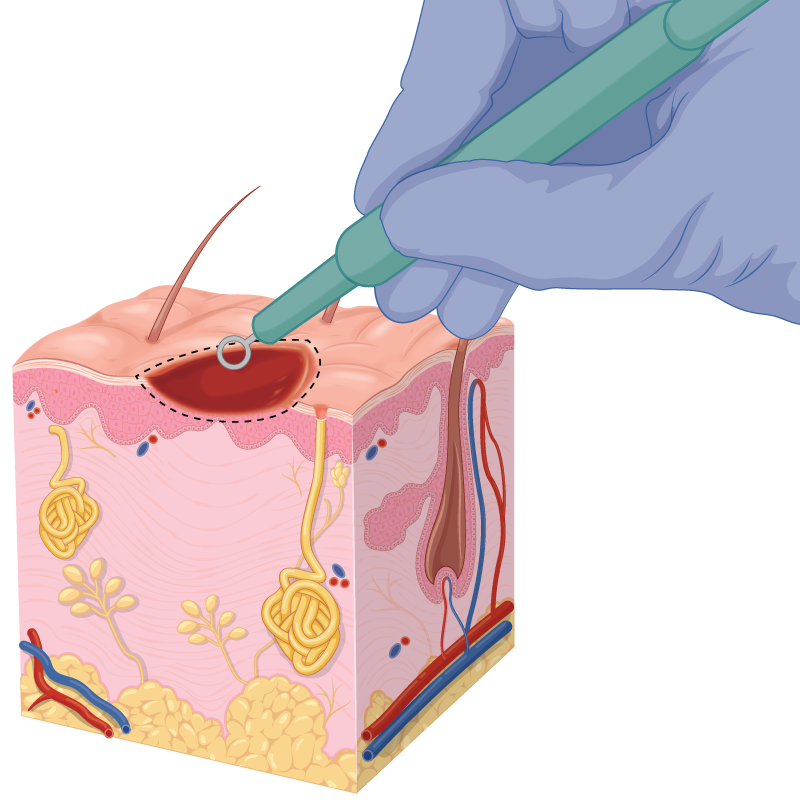
The procedure
- It is normally undertaken with a local anaesthetic.
- A sharp curette is used to debulk (remove) the tissue creating a broad but superficial wound.
- The wound is not stitched but is cleaned and a dressing is applied.
- You will be provided with a written information sheet that includes our after-hours contact number. While we don’t expect problems, we want to ensure that we are there for you should the unexpected arise.
Curettage & electrodessication
Curettage and electrodessication (also known as diathermy) are often called curettage and cautery (abbreviated as C&C). This is often used when treating superficial skin cancers or precancerous lesions. The intent is to reduce the risk of the cancerous lesion from returning.
- Curettage is immediately followed by electrodessication which uses heat to destroy a superficial layer of tissue at the base of the wound.
- The C&C may be performed 2-3 times to minimise the risk of recurrence.
Recovery process
After the procedure, there will be a superficial ulcer (depression) of the skin where the procedure was performed. There are no stitches to have removed. As a result, most people can continue with their normal activities with minimal disruption. The application of white soft paraffin may help reduce crust formation and improve the cosmetic outcome.
The wound will normally heal by granulating and forming an eschar (scab) over 4-6 weeks. Superficial curettages can heal without a scar, whereas a deep procedure would be expected to leave a scar that is broad and depressed. They may also leave a white discolouration of the skin. It is therefore best to avoid deep curettages in cosmetically sensitive areas.
As with all surgical procedures, there is a risk of bleeding and infection, however, this risk is low with curettage as the wound is superficial.